huffingtonpost.com: To End The Opioid Crisis, Doctors Must Acknowledge We Helped Create It
7/11/2018
I’m a physician who specializes in addiction medicine, which means I’ve been busy lately. Busy treating some of the millions of Americans affected by the opioid crisis. Busy advocating for my colleagues in primary care to do the same.
In lectures and workshops, I ask them to start prescribing medications to help treat opioid addiction. I tell them patients are dying — and have died — because they are unable to find providers willing to help them. I remind them that drug overdose is now the leading cause of death for adults under 50 and that a medication called buprenorphine, which they have the power to prescribe, can cut that death rate by more than half.
This is a crisis, I tell them. We must act.
Not infrequently, my colleagues — smart, compassionate, dedicated doctors, nurses and physician assistants — refuse.
They tell me they bought the pharmaceutical company line once already, back when primary care providers were told to take care of patients’ pain and then given no resources other than opioids to do so.
They tell me they were taught that opioids weren’t addictive if prescribed to a patient in pain.
They describe how they were taught, as I was, that they needed to ask all their patients, every time, if they hurt, where they hurt and how much.
It turns out providers often weren’t helping those patients; we harmed them. Maybe even killed them. We helped start the opioid epidemic. So no, they tell me, they will not buy the promise of a magic pill again.
I want to shake them and scream, “This is not the same thing!” Opioids for chronic pain often have only moderate efficacy and carry significant risks; buprenorphine saves lives and helps decrease risk of HIV infection. I want them to stop arguing and just prescribe it.
The overprescription of pain pills created a population of patients dependent on opioids, some of whom became addicted to the medication.
However, I also understand their concerns. I once had a large and loyal cohort of patients whose pain I treated with opioids, opioids and more opioids.
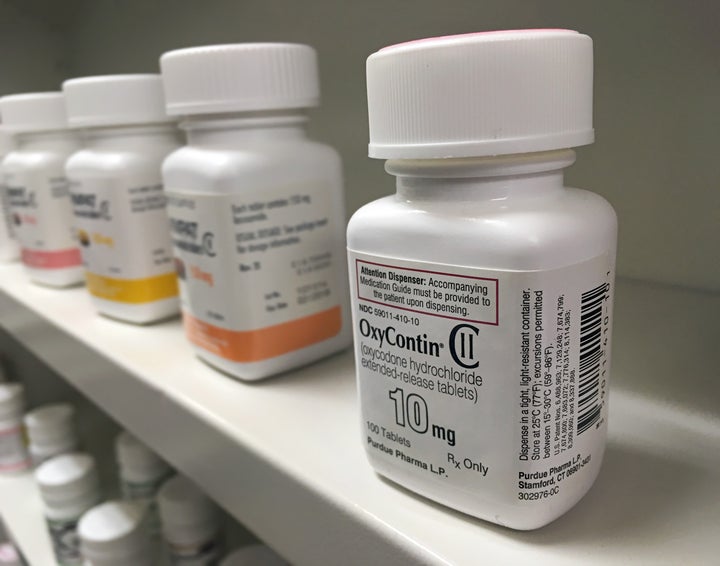
One middle-aged couple in particular sticks in my memory. He was soft and starting to bald; she was small, sad and always in pain everywhere. In rushed 15-minute appointments, I’d ask her to point to a pain scale consisting of cartoon faces in a line, ranging in order from happy painlessness to a face in such agony it was sobbing. She’d point to that last round head, and I’d again prescribe her OxyContin. The couple would thank me for being the doctor who finally understood her pain, finally understood that she needed help, relief and compassion.
But I didn’t understand. At all. I had received no training in the treatment of pain. I didn’t know if counseling would help.
I didn’t know which kinds of physical therapy, injections or surgeries my patients might need, whether those interventions worked or how to get any of it covered by insurers.
I didn’t know that persisting pain is often connected to depression, anxiety and trauma.
I didn’t know how to recognize addiction ― or how to treat it.
All I knew was that when I suggested my patient taper the OxyContin, she’d crumple in despair. And her soft husband would, like the Hulk, become monstrously large and angry, demanding I show some compassion, god damn it.
It’s possible my patient was addicted to opioids. It’s more likely she wasn’t and that she simply had few options for pain control besides those pills, which, at minimum, helped her mentally check out of her misery. She was desperate for relief, and I was desperate to be useful. She was just one of my many patients in pain, and I didn’t know the right thing to do, the wrong thing or where to get help. I also knew insurance wouldn’t cover most of the alternative treatments I might offer.
It wore me down. I began to hate my patients’ gratitude when I prescribed opioids and to resent their anger when I suggested tapering. I stopped listening, except in a cursory way. I met their needs, documented my exam and often otherwise tuned out. I also stopped being the kind of doctor I’d aspired to be. I thought about leaving the profession.